Answer of March 2025
For completion of the online quiz, please visit the eHKAM LMS website.
Clinical History:
A 62-year-old man present with left knee suprapatellar mass for months. MRI left knee with contrast and plain radiograph of left knee was performed.
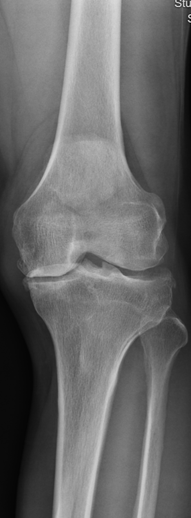
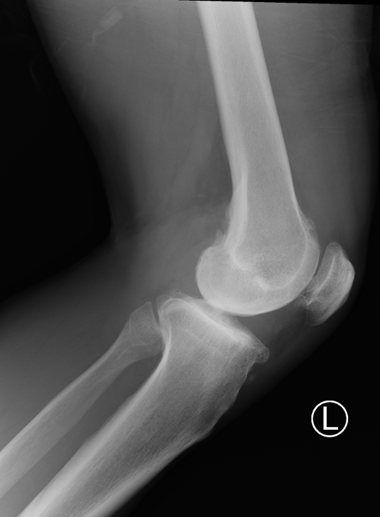
Plain radiographs of left knee:
MRI left knee with contrast
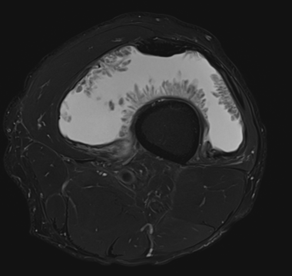
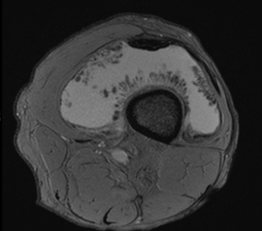
1) Axial T2 FS
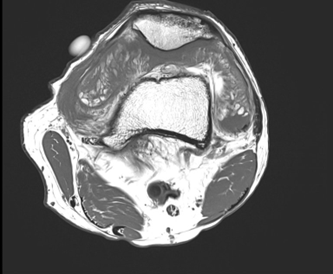
2) Axial T1
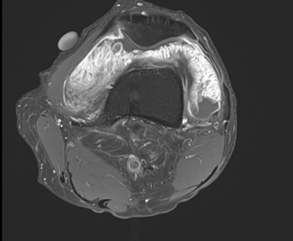
3) Axial SWI
4) Axia T1 FS post contrast
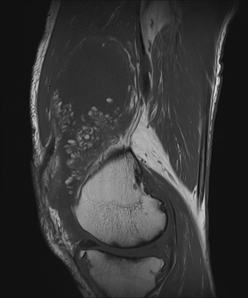
5) Sagittal T1
DIAGNOSIS:
Lipoma arborescens
IMAGING FINDINGS:
Lipoma arborescens is a rare, chronic and benign intra-articular lesion characterised by villous lipomatous proliferation of the synovium, commonly affecting patients between the fifth and seventh decade. It can occurs secondary to joint disease eg osteoarthritis, meniscal injury, trauma, arthritis, or chronic synovitis. The primary type (i.e. without secondary cause) is relatively rare. It most commonly involves knee joint particularly suprapatellar pouch. Other joint involvements such as the hip, elbow, shoulder, and ankle have been described. Bilateral joint involvements are very rare.
Patient usually present with insidious slowly progressive painless swelling of the joint, which persists for many years and is accompanied by intermittent effusions. On radiography, soft tissue opacity over involved joint e.g. suprapatellar pouch can be present. Degenerative changes can be present in case of secondary form. Important negative findings from radiographs eg absence of sclerosis, calcifications or erosions are important clued in the differentiating with pigmented villonodular synovitis (PVNS) and gouty arthropathy.
From, MR imaging, it shows high signal intensity frond-like projection on both T1- and T2-weighted images with signal suppression observed in STIR or fat saturation sequences. The absence of susceptibility artefact on gradient imaging differentiates this condition from PVNS. The remaining non-fatty component of hypertrophied synovium in the condition displays heterogeneous high signal intensity on T2 or STIR sequences and intermediate-to-low signal intensity on T1-weighted sequences. The thickened synovium often displays diffuse enhancement. Degenerative changes and meniscal tears can be noted as pathological factors contributing to the development of lipoma arborescens. The definitive diagnosis of arborescent lipoma is typically established through histopathological examination, obtained by synovial tissue biopsy or surgical intervention. Microscopic analysis reveals the presence of mature adipocytes infiltrating the subsynovial tissues, distinguishing it from other joint pathologies.
The treatment of lipoma arborescens is surgical or arthroscopic synovectomy which aimed at removing proliferative adipose tissue and restoring joint function. It is crucial to address and treat the underlying triggering factors. After surgery, the recurrence of the pathology is minimal.