Answer of July 2017
For completion of the online quiz, please visit the HKAM iCMECPD website: http://www.icmecpd.hk/
Clinical History:
A 37-year old lady with good past health complained of long-standing hoarseness and incidental polycythemia. Clinical findings revealed a significant finding. The patient was thus referred for CT neck and thorax to investigate for the underlying cause of this finding.
Diagnosis:
Patent Ductus Arteriosus associated with Left Vocal Cord Palsy
Discussion:
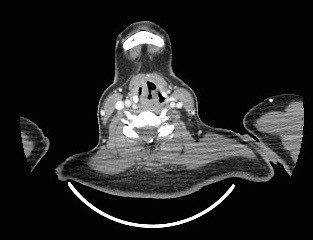
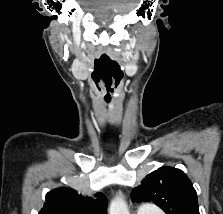
The CT neck of this patient reveals typical radiological features of left vocal cord palsy. The classical radiological signs of unilateral vocal cord palsy include ipsilateral piriform sinus dilatation, medial rotation and thickening of the aryepiglottic fold, ipsilateral laryngeal ventricle dilatation, and anteromedial displacement of the ipsilateral arytenoid cartilage with medial displacement of the posterior vocal cord margin. The combination of medialization of the posterior vocal cord margin and air distending the ipsilateral laryngeal results in the residual airway having a shape similar to a ship’s sail, known as the “sail” sign.
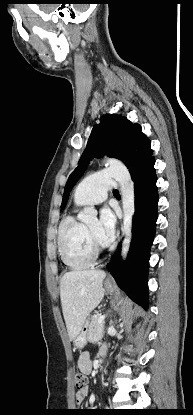
Patent ductus arteriosus is a normal connection of the fetal circulation between the aorta and the pulmonary artery. After birth, the ductus arteriosus normally closes functionally in the first 10-18 hours of life, and anatomically in 2-3 weeks. If it remains open beyond three months of life in preterm infants and beyond one year of life in full-term infants it is termed as persistent patency of ductus arteriosus because the incidence of spontaneous closure beyond these time limits is very low.
The clinical features of patent ductus arteriosus vary a lot. Patients with small PDAs can be asymptomatic. Patients with large PDAs may present with repeated lower respiratory tract infection, poor growth, failure to thrive, or heart failure. Patients with PDA undiagnosed until adulthood may present with heart failure, arrhythmia, and differential cyanosis limited to the lower extremities, indicating shunting of deoxygenated blood from pulmonary to systemic circulation.
Left recurrent laryngeal nerve palsy is rarely associated with patent ductus arteriosus but has been reported. The greatly dilated pulmonary artery in these patients resulted in compression of the left recurrent laryngeal nerve and produced a cardiovocal (Ortner's) syndrome.
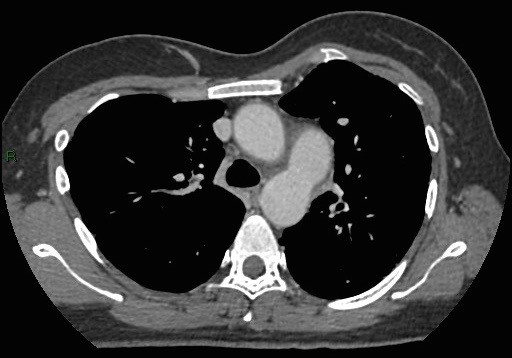
Another finding in the CT of this patient is the dilatation of pulmonary trunk and central pulmonary arteries. The patient was referred to Cardiology team. Echocardiography and cardiac catheterization were performed, which also found a large Patent Ductus Arteriosus, enlarged pulmonary artery with pulmonary hypertension suggestive of Eisenmenger physiology, dilated right atrium and right ventricle.